Glaucoma cannot be cured, nor can lost vision be replaced or regenerated. However, further visual damage can be prevented by special glaucoma medications (eye drops or pills), laser surgery, or other microsurgical procedures. For more information regarding glaucoma please see our main glaucoma center website page.
Glaucoma Medications
 A number of different glaucoma eye drops are available to lower the IOP. Most of the commonly used drops are dosed from one to three times per day. The drops work by either reducing fluid production inside the eye, or by increasing fluid outflow (drainage). Some of the drops also help to even out rises or fluctuations in IOP that can occur even at night, thereby leading to more level pressure control throughout the entire day. Eye drops can have side effects or interactions, so it is very important to inform your ophthalmologist of your medical conditions and of other medications you may be taking. Certain oral medications may also be used to treat glaucoma, although these are usually reserved for more severe cases or for short-term use.
A number of different glaucoma eye drops are available to lower the IOP. Most of the commonly used drops are dosed from one to three times per day. The drops work by either reducing fluid production inside the eye, or by increasing fluid outflow (drainage). Some of the drops also help to even out rises or fluctuations in IOP that can occur even at night, thereby leading to more level pressure control throughout the entire day. Eye drops can have side effects or interactions, so it is very important to inform your ophthalmologist of your medical conditions and of other medications you may be taking. Certain oral medications may also be used to treat glaucoma, although these are usually reserved for more severe cases or for short-term use.
Glaucoma Laser Surgery
Lasers have a number of applications in glaucoma treatment as described below. All laser procedures are brief, in-office or outpatient treatments.
Selective Laser Trabeculoplasty (SLT)
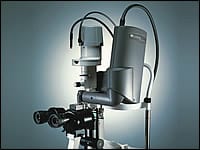 A low power laser with a very short pulse of light, the SLT laser is applied directly to the trabecular meshwork to enhance or stimulate its normal drainage function. The laser causes a drop in IOP without cutting tissue or creating new holes or openings in the eye. SLT treatment offers many advantages to patients. It can be performed as an initial treatment instead of eye drops for patients who cannot tolerate medications or who desire fewer or no medications. It can be added to drops as a supplemental treatment for greater IOP lowering when necessary, allowing for less complex medical regimens. There are no systemic side effects. It is a safe, office-based procedure, performed simply with a drop of anesthetic in the eye. It is reimbursed by medical insurance. In some patients, the IOP lowering effect of the SLT laser may wear off over time, requiring a retreatment with the laser or a different therapeutic approach. SLT may be performed prior to cataract surgery in patients with coexisting glaucoma and cataract to maximize the chances of good IOP control with less need for glaucoma medications following cataract surgery.
A low power laser with a very short pulse of light, the SLT laser is applied directly to the trabecular meshwork to enhance or stimulate its normal drainage function. The laser causes a drop in IOP without cutting tissue or creating new holes or openings in the eye. SLT treatment offers many advantages to patients. It can be performed as an initial treatment instead of eye drops for patients who cannot tolerate medications or who desire fewer or no medications. It can be added to drops as a supplemental treatment for greater IOP lowering when necessary, allowing for less complex medical regimens. There are no systemic side effects. It is a safe, office-based procedure, performed simply with a drop of anesthetic in the eye. It is reimbursed by medical insurance. In some patients, the IOP lowering effect of the SLT laser may wear off over time, requiring a retreatment with the laser or a different therapeutic approach. SLT may be performed prior to cataract surgery in patients with coexisting glaucoma and cataract to maximize the chances of good IOP control with less need for glaucoma medications following cataract surgery.
Laser Iridotomy
In this procedure, a tiny hole is made in the peripheral iris to break an attack of acute angle closure glaucoma, or to prevent angle closure in patients with narrow anterior chamber angles (primary angle closure glaucoma suspects). Argon or YAG lasers are typically used for these treatments.
In laser iridoplasty an argon laser is used to slightly shrink the tissue of the mid-peripheral iris in order to pull it out of the drainage angle, to remove adhesions that may have already developed, or to prevent adhesions between the iris and trabecular meshwork that can lead to chronic angle closure glaucoma.
Endoscopic Cyclophotocoagulation (ECP)
In this novel procedure, a tiny, delicate probe containing an argon laser delivery system is placed inside the eye. Through a fiberoptic line that is part of the probe, the surgeon can visualize the inside of the eye on a video camera. The laser light is applied to the ciliary body, the structure inside the eye that makes aqueous fluid. The laser energy causes a reduction in fluid production and a lowering of IOP. ECP is most commonly performed in conjunction with cataract surgery in patients that also have glaucoma.
Diode Cyclophotocoagulation (CPC)
Laser energy is delivered to the ciliary body through an external approach with a special probe on the surface of the eye. This treatment is often reserved for advanced stages of glaucoma that may be difficult to control by other means, or for eyes with high pressure that are poor candidates for more conventional surgery.
Glaucoma Microsurgery
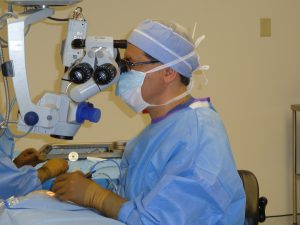 Different types of microsurgical interventions are available for IOP control and maintenance of vision, when medications or laser surgery do not provide sufficient control or are otherwise not appropriate.
Different types of microsurgical interventions are available for IOP control and maintenance of vision, when medications or laser surgery do not provide sufficient control or are otherwise not appropriate.
iStent® Trabecular Micro-Bypass

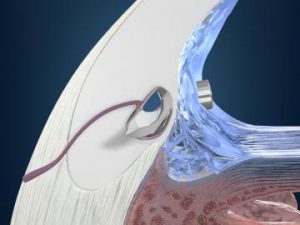
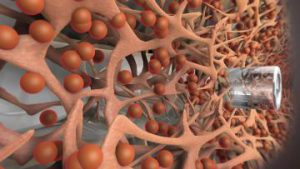 iStent® improves your eye’s natural fluid outflow to safely lower eye pressure. It is placed in your eye during cataract surgery for the reduction of intraocular pressure in patients with mild to moderate open-angle glaucoma. iStent is designed to create a permanent opening in your trabecular meshwork, and works continuously to improve the outflow of fluid from your eyes to help control eye pressure. Made of surgical-grade titanium, the stent is placed in an internal area of the eye known as Schlemm’s canal to re-establish a more normal flow of fluids within the eye. It is so small that you won’t be able to see or feel it after the procedure is over.
iStent® improves your eye’s natural fluid outflow to safely lower eye pressure. It is placed in your eye during cataract surgery for the reduction of intraocular pressure in patients with mild to moderate open-angle glaucoma. iStent is designed to create a permanent opening in your trabecular meshwork, and works continuously to improve the outflow of fluid from your eyes to help control eye pressure. Made of surgical-grade titanium, the stent is placed in an internal area of the eye known as Schlemm’s canal to re-establish a more normal flow of fluids within the eye. It is so small that you won’t be able to see or feel it after the procedure is over.
Trabeculectomy
A procedure where a new drainage system is created with the patient’s own eye tissues. Aqueous fluid is rerouted from the blocked passageways to a new drainage site which results in lowering of the eye pressure. The standard glaucoma operation, trabeculectomy surgery has undergone refinements and modifications to improve the success rate, including the use of anti-scarring agents, new suture materials, and tissue handling techniques to enhance proper fluid outflow.
Aqueous Shunts
These are devices that are implanted in the eye to bypass the internal obstruction and to shunt the aqueous fluid to a new collecting system.
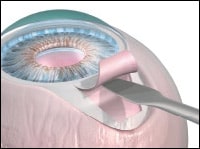
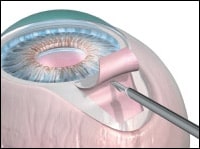
Schlemm´s Canal Surgery
Schlemm´s Canal is the channel that links the trabecular meshwork inside the eye with the venous collecting system on the surface of the eye, which is where the aqueous fluid eventually drains. For many years, the opening or tearing of this canal to facilitate the flow of aqueous out of the eye has been the mainstay of glaucoma surgery in congenital glaucoma (glaucoma in babies or small children). Similar techniques and concepts are now being evaluated and refined to treat adult glaucoma as well.
Berkshire Eye Surgery Center
Berks Eye completes most Glaucoma procedures at Berkshire Eye Surgery Center, a fully equipped eyes-only ambulatory surgery center that provides convenience and comfort for our patients. Our center is accredited by the Accreditation Association for Ambulatory Health Care (AAHC), Medicare certified, and specially designed to accommodate Cataract, Glaucoma, Eyelid, and Laser procedures. To schedule an appointment for Glaucoma surgery, first schedule a consultation at our facility in Wyomissing to see if you are a good candidate for treatment.

 1802 Paper Mill Road, Wyomissing, PA 19610
1802 Paper Mill Road, Wyomissing, PA 19610

